Maternal Mortality Rate in the United States: A Persistent Crisis Demanding Urgent Action
Overview
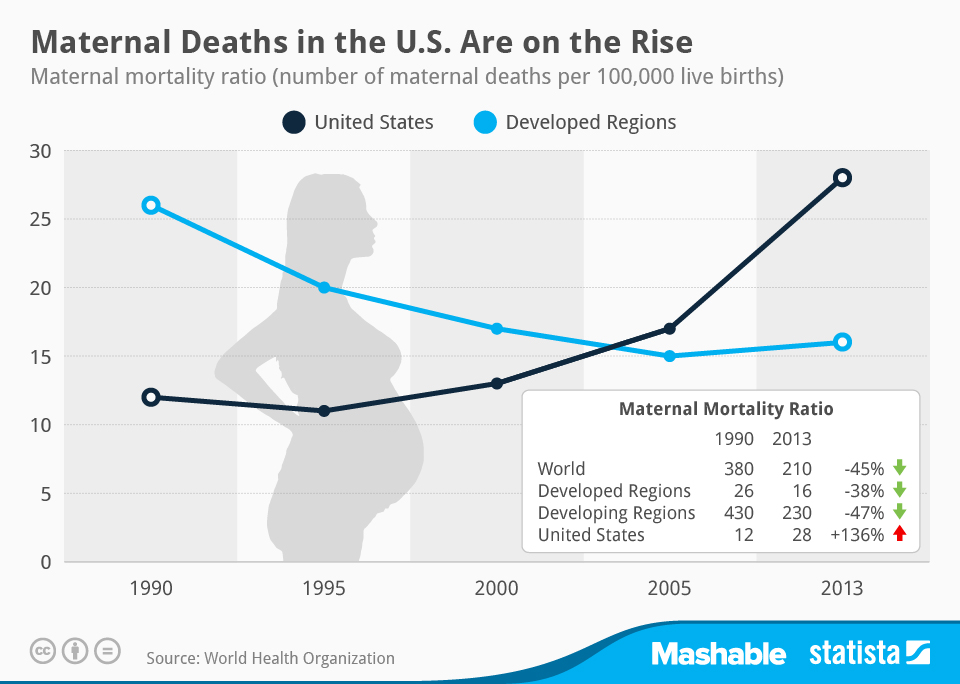
The tragic and urgent global issue of maternal mortality is the death of a woman during her pregnancy or within 42 days of the conclusion of her pregnancy. Maternal mortality rates have decreased significantly worldwide, yet the United States is still experiencing a chronic problem in this area. When compared to other industrialized nations, the United States has startlingly high rates of maternal mortality, even though it is one of the richest countries. This article explores the causes of the high maternal death rate in the US and highlights the pressing need to resolve this persistent issue.
I. The Disconcerting Situation of Mother Death in the US
- Relative to Other Developed Nations
When it comes to rates of maternal mortality, the United States has continuously fallen short of other industrialized nations. Surprisingly, the United States has more than twice the maternal mortality rate of many European countries, making it the highest among all developed nations. Considering the improvements in healthcare and medical technology accessible in the United States, this difference is even more concerning.
- Disparities by Race
Women of color are disproportionately affected by the maternal mortality rates in the United States. Pregnancy-related deaths account for two to three times as many deaths for Alaskan Native, African American, and Native American women as for White women. This discrepancy highlights structural problems that need to be addressed, such as racial bias in the medical field, restricted access to high-quality care, and a higher prevalence of chronic illnesses in underprivileged populations.
II. Factors Associated with High Rates of Maternal Mortality
- Insufficient Access to High-Quality Medical Care
Inadequate access to high-quality healthcare is one of the major causes of the high maternal mortality rate in the United States. Many women confront obstacles like no health insurance, few healthcare facilities in remote locations, and excessive healthcare prices, especially those from marginalized populations. These obstacles lead to inadequate or delayed prenatal care, restricted access to obstetric emergency services, and a higher chance of undiagnosed problems.
- Systemic racism and implicit bias
Maternal mortality rates among women of color are disproportionately high due in large part to systemic racism and implicit bias. Healthcare professionals’ implicit prejudices may result in poor treatment, a delay in diagnosing conditions, and disdainful attitudes about the issues and suffering that women of color face. Reducing racial inequalities in maternal death rates requires addressing implicit bias and fostering cultural competency within healthcare institutions.
III. The Need for Quick Action
- Improved Reporting and Data Gathering
Enhancing maternal mortality data collection and reporting is essential to determining the scope of the issue and the best course of action. Establishing standardized procedures for gathering data, improving reporting systems, and conducting thorough examinations of maternal fatalities are crucial for creating evidence-based policies and interventions that specifically address the requirements of vulnerable groups.
- Greater Healthcare Access
Reducing maternal mortality rates requires increasing access to healthcare services. Affordable healthcare coverage for all women, particularly those from underprivileged communities, should be the main goal of policy. Enhancing the availability of telemedicine services and expanding the number of medical institutions, especially in remote regions, might facilitate better access to emergency obstetric care, postpartum assistance, and prenatal care.
- Taking Social Determinants of Health into Account
The social determinants of health need to be addressed in order to address the root causes of maternal mortality. Inequalities in housing, food, education, and racial inequality are among the issues that need to be addressed. Maternal mortality rates can be decreased and overall health outcomes for mothers can be improved with comprehensive interventions that focus on these social variables.
- Training in Cultural Competence and Anti-Bias
In order to recognize and meet the specific requirements and difficulties encountered by a variety of patient populations, healthcare workers need to undergo continual training in cultural competency. Programs for medical education should include anti-bias training in order to address unconscious biases and advance fair treatment for all women.
In summary
There is an urgent need to address the crisis posed by the United States’ chronically high maternal mortality rate. We can significantly lower maternal death rates by addressing the underlying causes, which include systematic racism, implicit bias, and limited access to healthcare. Working together, governments, healthcare professionals, and communities must develop comprehensive plans that put maternal health first and guarantee that no woman dies during pregnancy or childbirth from avoidable causes. We can only build a future where every woman gets the support and care she needs to have a safe and successful pregnancy by working together.
